In this PrOPEL Hub blog, Professor Sara Connolly summarises findings from the new International Public Policy Observatory (IPPO) report and highlights the need for greater investment in NHS staff wellbeing.
Poor mental health and wellbeing costs the NHS an estimated £12.1 billion a year, according to analysis by the University of East Anglia and RAND Europe in a new The International Public Policy Observatory (IPPO) report. Saving the equivalent of just 10 per cent of lost days each year, could pay for more than 34,000 nurses and 17,000 doctors, according to the report. It finds that poor mental health among staff contributes to chronic staff shortages, poor staff retention and record patient waiting lists.
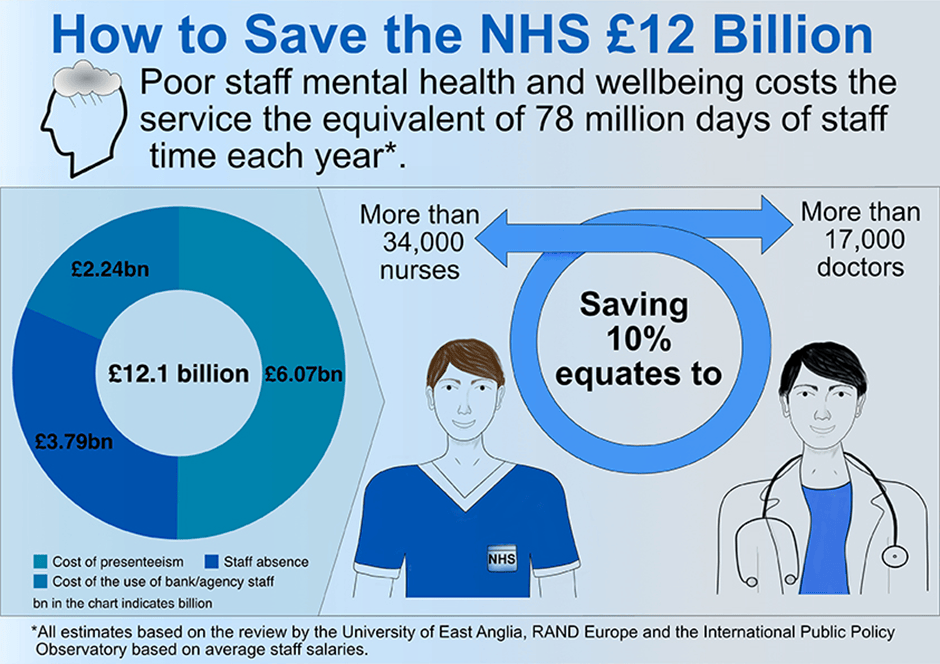
The analysis illustrates the very significant costs to the NHS of not acting to invest in their staff health and wellbeing. It makes the case that the NHS needs to spend more on staff wellbeing in order to save more. Investment in staff wellbeing can improve productivity and patient care, and can also lead to savings which can be re-invested into the health service which in turn will also lead to better patient outcomes.
Recommendations from the review include:
· Put protection of NHS staff health at the core of operational plans, governance, and strategies. For example, as part of the NHS People Plan, the NHS Long Term Plan and the NHS Five Year Forward View.
· Make staff wellbeing a core focus in inspections and reviews by regulators such as the Care Quality Commission, the General Medical Council and the Nursing and Midwifery Council.
· Improve NHS governance principles as applied to the wellbeing of NHS staff, such that accountability for the health of the NHS workforce is clearly defined and well understood.
· In addition to the NHS Staff Survey there is a need for shorter, more frequent and operationally focused tools to monitor the wellbeing and mental health of staff on a regular basis. Here the NHS should follow the example of other organisations – notably the British military – which conduct longitudinal monitoring of personnel, through an agency funded by, but independent of, the military itself.
· Sustained, ring-fenced investment at scale is required to reduce costs in the long term. Money saved should be spent on more staff to help reduce the levels of poor mental health.
The report highlights that there are numerous practices the NHS can introduce to prevent problems with staff wellbeing happening at source – for example management development and enhanced access to flexible working schedules. The scale of the problem means there is no silver bullet or quick fix, off-the-shelf solution. Rather, a strategic and systemic approach is needed that brings together a range of practices that simultaneously promote patient care and NHS staff wellbeing – these are compatible not mutually exclusive outcomes.
The report by the IPPO, UEA and Rand Europe is available here.



